Worried About How to Deal with Pain at Home?
Back to the Table of Contents
Patients about to go home from the hospital are often worried about how to deal with pain. (These fears are also felt by patients who are not in pain or whose pain is occasional.) If they are being given medication by their nurses and doctors to relieve pain, they often wonder: "Who will give me the medicine at home?" "What if I run out of medicine?" "Suppose I should need an injection?" "What if I'm alone and the pain gets worse?" They might also wonder: "If I start taking medications frequently, won't I become addicted?" "Will I reach a point where the drugs won't work any more?"
The first important point to remember is that most pain can be relieved. There are many medications available, and one or more of them will certainly help to relieve your pain.
Communicate About Pain to Your Doctor
Back to the Table of Contents
Usually all it takes to get pain under control is for you to note all the ways in which your medicine affects you, and to tell your doctor what you have observed. Your family members should also give their impressions of the way your medications work With this information, the doctor can make minor changes in dosage or type of medication that may make all the difference. If you find that one medicine is not working, there are always others that will probably help you.
Acute vs. Chronic Pain
When we describe pain, we have to decide whether it can be called chronic or acute.
Chronic pain is with you most of the time. Your medicine may relieve it for a while, but it usually comes back. This kind of pain needs continuous treatment; round-the-clock medication you would take in the same way as an antibiotic. There may be chronic pain with certain types of cancer. This is why you will be given a medication schedule. If your pain changes so that it is breaking through despite the treatment, let your caregivers know so that an adjustment can be made quickly.
Acute pain is a pain which seems new to you. You may have had it before, but when it comes, it is sudden and severe. Anyone who has had appendicitis is familiar with acute pain. When your pain is of this type, you should notify your physician. It doesn't necessarily mean that anything is seriously wrong with you. It may be a sign of tension from fear or worry, or it might be a minor problem caused by something such as constipation. But your physician should investigate it to make sure.
Pain is a very complex event in the body. It is caused by a mixture of emotional and physical factors. It is often made worse by tiredness. Even so, some patients whose pain is severe are still able to be comfortable because they have worked out a good schedule for their medications and either know how to handle it themselves or have a dependable person who can administer them.
In order to overcome pain, you should remember that you are the expert. On the other hand, although pain is a private and personal thing, it will help you to share your feelings with those close to you, as well as with your physician.
-
Telling your doctor that the pain medication doesn't work is the first step in taking control; but giving the doctor some specific details will help in finding a solution. The more information you can give your doctor, the better.
Try asking yourself these questions:
- What does the pain feel like? Is it sharp, dull, intermittent, stabbing?
Where is the pain?
What makes the pain go away? Changing positions? A different activity? Medication? A back rub? A hot bath?
How long does it take my medicine to start working?
How long does the relief last?
Does the pain interrupt my sleep?
Have I noticed any side effects?
-
You can write down the answers before your next visit with the doctor, and even keep a daily or hourly record. This will present the information in a clear form, and help the doctor help you.
Side Effects of Pain Medications
Back to the Table of Contents
Constipation
Pain medications containing narcotics usually affect the digestive system. But there are ways of dealing with the side effects, and they shouldn't prevent you from using a drug which successfully relieves pain. Constipation is a common problem. Stool softeners, laxatives, or enemas may be needed daily for as long as you receive the narcotic. Bulk laxatives (such as Metamucil®) are one type to avoid when taking narcotics; they may cause severe constipation rather than relieve it. Treating constipation should be done with care, so you will not have more serious complications, such as stool impactions (a severe form of constipation).
Nausea
Another common side effect of pain medication is nausea. This too can be eased by anti-nausea medications, such as Dramamine®, Compazine®, Tigan®, and others. If you are having any unpleasant side effects from your medication, be sure to tell your doctor. But, never stop taking your medication without first checking with your doctor.
Types of Medications
Back to the Table of Contents
 As you know, medications come in different forms: pills, liquids, rectal suppositories, and injections. Before you leave the hospital, you should ask your physician about the type of medication you will be taking home with you. Then you must learn now to take the medicine, or your family helpers must learn how to give it to you.
As you know, medications come in different forms: pills, liquids, rectal suppositories, and injections. Before you leave the hospital, you should ask your physician about the type of medication you will be taking home with you. Then you must learn now to take the medicine, or your family helpers must learn how to give it to you.
Usually your doctor will send you home with the same pain medication you have been taking in the hospital. If you will be taking a different type, your doctor will probably have started you on it before you are sent home, to see how well it works and what side effects it may have on you. It is better to have this trial in the hospital. There you can be observed by the nursing staff, and become secure with the medicine.
Learn to Administer Your Own Medication
Remember! You can learn to give yourself just about any pain medication you might need. And if this is not possible, your family can help. Most people are afraid to give themselves injections; but remember that many diabetics do this every day. By learning to overcome these fears, and learning to manage a daily medication program, you can free yourself from the hospital and start to control the pain yourself.
Types of Medications
If you will be taking pills or tablets home with you, ask the nurse for a stack of plastic medicine cups. These are handy for setting out each dose, especially those you may have to take through the night.
If you have difficulty swallowing, pills may be crushed by placing them in a plastic bag and gently crushing them with a spoon. Add the crushed pills to a spoonful of soft food, such as custard, applesauce, or cereal. You may also dissolve the crushed mixture in a small amount of water or juice. Don't use too much liquid, though, as you may not be able to finish it and get all of your medication.
Small plastic cups are also handy for taking liquid medications. Some have markings on the side to let you measure out the correct amount. Liquid medications can be mixed with juices to make them more palatable.
Suppositories for Pain
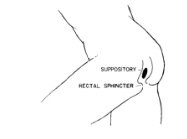 Rectal suppositories are easy to use. Simply remove the foil wrapper, lubricate the tip with K-Y Jelly® or water, and insert it into the rectum using your index finger. It must be pushed up past the rectal sphincter, or muscle, usually as far as your finger will reach.
Rectal suppositories are easy to use. Simply remove the foil wrapper, lubricate the tip with K-Y Jelly® or water, and insert it into the rectum using your index finger. It must be pushed up past the rectal sphincter, or muscle, usually as far as your finger will reach.
Injections for Pain
Injections are often frightening to patients and their families. Many people dislike them and are horrified by the thought of giving one to themselves or to someone they love. Any nurse will tell you how nervous she felt when giving her first injection. But keep in mind that injections give many patients excellent relief from their pain.
The technique of giving an injection is easy to learn if you give it a chance (and is explained clearly in The Steps of Giving an Injection). You will learn how to measure the medication and draw it into the syringe; how to choose the right spot for an injection; and how to prepare the skin and inject the medication. Arrange to have someone in your family, or the person who will be caring for you at home read this section as well. It is important that someone else knows the technique; you should not have to worry about who will be giving you injections at home.
You and the others who will be responsible for your injections will need practice before you feel able to give a shot safely and comfortably. After you have practiced, perhaps on an orange, have a nurse help you with your first real injection. Remember, you can learn to give an injection, even to yourself! Knowing that you can give a shot will give you confidence that you can control pain.
Pain medications are injected just below the outer skin (subcutaneously) or deep into the muscle tissue (intramuscularly). Generally speaking, medications which are irritating to the skin or which are designed to act quickly are injected intramuscularly. Non-irritating medications are often injected subcutaneously.
Choosing the correct place for an injection is an important decision, and will be made by your nurse or physician. He or she will advise you of the best place for each of your injections.
Pain Medication Do's and Don'ts
Back to the Table of Contents
- Here is a brief list of Do's and Don'ts, which apply to you no matter which medicines you are taking for pain.
Do's
- Know the name, dosage and side effects, if any, of your medications.
Have a responsible member of your family learn the timing of your medications and the way you take them.
Follow the instructions on the label carefully. Many medicines for pain are ordered PRN; this means you take them as needed; take these medications before your pain gets severe. They are more effective at the start of pain.
Reorder your medication before you run out of it.
Remember that narcotics require a written form from your physician, so it is important to call for refills during office hours.
Know the name and phone number of your pharmacy.
Triple check to make certain you have the right medications before taking them. If your eyesight is poor, use a magnifying glass to read the label.
Keep a written list of all the medications you are currently taking. Include on this list any medications you have taken in the past which have given you unpleasant side effects, and any medications to which you are allergic. Carry a copy of the list in your wallet or purse. Bring it with you when you visit your doctor, or if you return to the hospital.
- Medication Record

-
Keep a careful record of each time you take your medicine, including the date and time (AM or PM).
- Dont's
- Transfer drugs from one container to another.
Take medications in the dark-read the labels.
Leave medications within easy reach of children.
Stop taking medications without notifying your doctor.
Neglect to notify your doctor if your medication is not relieving your pain.
Change your medication schedule without first checking with your doctor.
- To conclude, pain is a complex experience with both physical and emotional factors. Medication is just one way of relieving pain. See the sections on recreation, massage and meditation, which are also helpful in relieving pain.
Learning to control your pain means making careful observations about the way you experience it, when you experience it, and the effects your various medications have on it. Your family should also participate in making these observations. If this information is presented clearly to your physician, the types of medication and dosages can be adjusted to fit your needs for pain relief.
Once the medication has been decided upon by your physician, you and your family will only need a little practice and you will be able to take control of your pain relief program.
Graphics courtesy of the U.S. Department of Health and Human Services, National Institutes of Health
|

 As you know, medications come in different forms: pills, liquids, rectal suppositories, and injections. Before you leave the hospital, you should ask your physician about the type of medication you will be taking home with you. Then you must learn now to take the medicine, or your family helpers must learn how to give it to you.
As you know, medications come in different forms: pills, liquids, rectal suppositories, and injections. Before you leave the hospital, you should ask your physician about the type of medication you will be taking home with you. Then you must learn now to take the medicine, or your family helpers must learn how to give it to you.
 Rectal suppositories are easy to use. Simply remove the foil wrapper, lubricate the tip with K-Y Jelly® or water, and insert it into the rectum using your index finger. It must be pushed up past the rectal sphincter, or muscle, usually as far as your finger will reach.
Rectal suppositories are easy to use. Simply remove the foil wrapper, lubricate the tip with K-Y Jelly® or water, and insert it into the rectum using your index finger. It must be pushed up past the rectal sphincter, or muscle, usually as far as your finger will reach.
