|
Fifth Dimension Site Map Search Contact Us |
|

|
Cancer Risk Assessment Introduction |
Introduction
Back to the Table of Contents
People diagnosed with cancer often say that initially they had a feeling of disbelief. Some say they felt numb, heard a ringing in their ears, or felt that their "mind turned to cotton candy." Still others, particularly those who have one or more close relative with cancer, report they almost had a sense of relief when they heard their diagnosis "now that the wait for cancer was over."
Whatever your initial feelings, you probably now have many questions, among them:
- What leads to the development of a cancer cell
- Your risks of a second cancer
- The risks of cancer to your children or other relatives
- Whether genetic testing might play a role in helping you and your family make health care decisions.
You might wonder whether it is wise to inquire about these areas, in case you learn something that would be further cause for concern. Rest assured that the material in this program is unlikely to upset your peace of mind. It is designed to help you and your family make decisions that will enable you to be as safe as possible and to feel safe.
Where Does Cancer Come From?
Back to the Table of Contents
Many people are surprised to learn that most cancers are not hereditary. That is, they do not run in families and are not due to genetic material that a person inherits from his or her parents. Even though most cancers are not hereditary, in considering how cancers arise, we need to consider the genes.
Formation of Non-Hereditary Cancers
Back to the Table of Contents
A person's genes are composed of long strings of chemicals. Amazingly, the chemicals in a gene have the ability to:
- reproduce themselves and
- make the chemicals that cause the body to grow and develop.
The genes are on the chromosomes, like electrons strung along an electrical wire. In Figure 1 below is a photograph of one woman's chromosomes. The bands you see are produced by different concentrations of chemicals along the chromosomes. They are used to distinguish between chromosomes. By convention the chromosomes are numbered: 1 and 2 are the largest and 21 and 22 the smallest. Women have two X chromosomes; men have one X and one Y chromosome.

A person inherits two copies of each gene: one from the mother and one from the father. So, as you can see in Figure 1, there are two copies of each chromosome. All of these chromosomes are present in most of a person's cells. This means that all of the chemicals needed to make a new human are present in most cells. Suppressor genes, which stop certain other genes from acting are one of the ways that a colon cell, for example, is able to produce only the chemicals needed to make a colon cell, even though the genes to make other cell types are present in colon cells. In the same way, a breast cell contains all of the genes needed to make a whole person. Suppressor genes in the breast are one way the cell keeps all genes except those needed for breast function from working. It's as if there were a complete piano in each cell. And, in each of the different cell types, only certain keys are allowed to function. So, a breast cell makes only the chemicals needed for breast cell growth and maintenance and a colon and other cells do the same for their cell type.
As long as suppressor genes function normally, all goes well. If, however, suppressor genes are damaged or lost, they are no longer available to maintain order. As a result, a cell may begin to divide in an unusual way. If more and more suppressor genes don't work, the division process may become more and more unruly, resulting in the loss of more and more genes. In time, a cancer cell may be formed. This process is shown in Figure 2 below for the formation of a non-hereditary colon cancer cell. As you can see, it's like the straw that breaks the camel's back: once enough suppressor genes are not working, the cell can become a cancer cell.
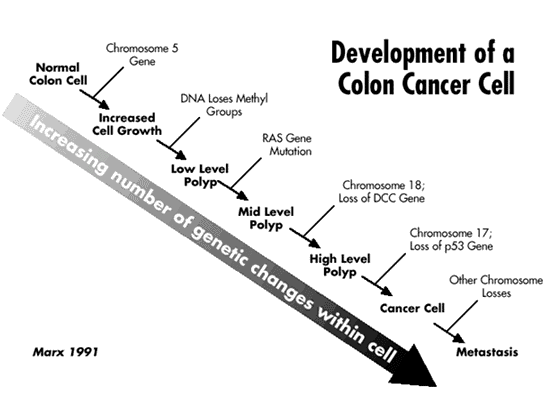
The changes shown in Figure 2 are known to occur in the formation of a non-hereditary colon cancer cell. All of the genetic changes needed to produce a cancer take place after conception in a single cell and its descendents, so it takes time for all of the changes to accumulate in one cell. That's probably why most non-hereditary cancers are diagnosed at older ages, not younger ages.
You can see now why cancers are said to be genetic - they are due to changes in the genes. Importantly, however, most cancers are not hereditary, since the changes occur in genes that are in a non-egg or non-sperm cell. All of the changes occur after conception. For a cancer to be hereditary, at least one genetic change (mutation) must be inherited through the egg or the sperm. That is, the genetic change is present at the moment of conception. The formation of hereditary cancer cells is discussed in a later section.
Environmental Agents
Back to the Table of Contents
Most cancers are not due to hereditary factors, so you might expect that it would be possible to screen an individual's environment, pinpoint any carcinogens that are present, and then remove them, reducing a person's cancer risk. Actually, the situation is more complex. While it is known that certain agents, such as exposure to high doses of X-rays at a young age, high levels of arsenic, asbestos, cigarette smoke, etc. increase the risk of cancer in groups of people exposed to these agents, individual levels of susceptibility differ, even within the same family.
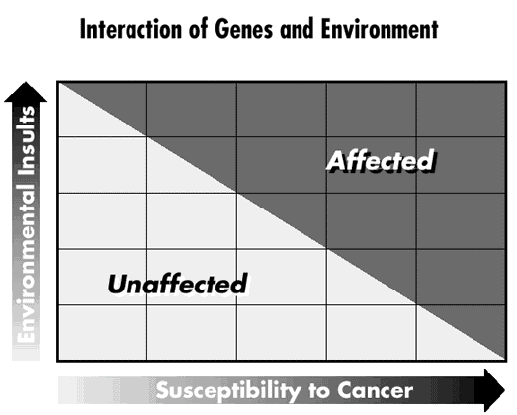
Figure 3 above shows how the interaction between a person's genes and the environment influences the chance of developing a cancer. As you can see, some individuals have a genetic make-up that makes them very susceptible to the products of cigarette smoke (bottom line on the right). Even small exposures will increase their cancer risk. Others, on the lower left side of the diagram, can tolerate a great deal of this carcinogen before they develop a cancer. Scientists are still studying how much of a particular chemical a population can tolerate in safety. It is important to remember as you read the results of studies that they tell you about population risks, not individual susceptibilities. The two may differ.
At the present time, much of the environmental cause of cancer remains unknown. Even less is known about an individual's own susceptibilities. This is likely to change, as more is understood about the genes, the products they make, and the role that the various genes play in making us, as individuals, susceptible or resistant. Another fast growing field has to do with genes that act to repair genetic damage that occurs due to every day living and to exposure to carcinogens.
Formation of Hereditary Cancers
Back to the Table of Contents
Fewer than ten percent of most cancers are thought to be due to strong hereditary factors. Strong hereditary factors that increase cancer risk are more likely to be found in families that have:
- Individuals diagnosed with cancer at a younger than expected age (for example, breast cancer in the 40's or prostate cancer in the 50's)
- Three or more cancers on once side of the family
- Three or more generations affected with cancer
- Individuals diagnosed with two or more cancers (but not a metastasis or spread from a cancer to another part of the body).
Not all families in which the cancers are due to strong hereditary factors will have these elements. And, families with none of these elements may still have hereditary cancer. For this reason, if you have questions about the cancer risk in your family, it is important to consult a geneticist who has experience in this field. As you will read in a later section, genetic testing can sometimes help to distinguish those who have hereditary risks from those who do not.
Second Cancers
Back to the Table of Contents
After a diagnosis of cancer, you may wonder how likely you are to develop a second one. A true second cancer is called a new primary. It is different from a metastasis, which is a spread of the first cancer to another part of the body. Usually doctors can tell the difference between a second primary and a metastasis by looking at the cancer cells under a microscope. In this section second primary cancers are discussed.
Second primary cancers are rare. Generally speaking, individuals with a strong family history of cancer have a higher chance of developing a second primary than those who have no family history of cancer. Genetic testing is sometimes useful in identifying people who have an increased risk of a second primary. Some of the types of families in which second primaries are more likely to occur are discussed in the next section.
Cancer Syndromes
Back to the Table of Contents
A syndrome is a collection of symptoms or diseases found in a person or a family. Scientists are learning more about changes in genes (called mutations) that increase the risk of cancer. Individuals who inherit some of these mutations have an increased risk of several cancers. For example, in some families the risk of breast and ovarian cancer is increased, while in other families risks of other cancers are higher. Two examples of cancer syndromes follow.
Breast Cancer Genes 1 and 2 (BRCA1 and BRCA2)
Back to the Table of Contents
The BRCA1 gene is on chromosome 17. BRCA2 is located on chromosome 13. A woman who inherits a mutation in either of these two genes has an increased risk of both breast and ovarian cancer. That is, the same genetic change results in an increased risk of these two cancers. In some families there is also an increased risk of pancreatic cancer, colon cancer, melanoma, and other cancers, but the risk of these cancers if far lower than the risk of breast and ovarian cancer.
Hereditary Non-Polyposis Colon Cancer (HNPCC)
Back to the Table of Contents
HNPCC stands for Hereditary Non-Polyposis Colon Cancer. Individuals who inherit a mutation in one of several genes have an increased risk of colon, uterine, stomach, ovarian and other cancers. Breast cancer risk also appears to be increased in some families with an HNPCC mutation, but the risk is lower than that of the cancers just mentioned.
Risk To Relatives
Back to the Table of Contents
In most families, even when several cancers are present, the cancers are not due to strong hereditary factors, so relatives are generally not at increased risk, unless there is a strong environmental agent present. This section discusses risk when a cancer syndrome is present and an individual's close relative, such as a mother, father, sister or brother has cancer that is hereditary. Scientists are still studying the precise cancer risks in these families. At present the information about risks is based on small numbers of specially selected research families, so the risks as now known are preliminary.
We do know that each of the close relatives of a person diagnosed with cancer has a 50% chance of inheriting a mutation that increases cancer risk. As you saw in Figure 1 individuals receive two copies of each of the genes that are not on the X and Y chromosomes. This means that each of a person's cells, with the exception of the egg and sperm cells has two copies of each gene (again, with the exception of genes on the X and Y chromosomes). Egg and sperm cells contain only one of each chromosome and so one of each gene. Therefore, as you can see in Figure 4, a parent who has a mutation that increases cancer risk on one chromosome will make two types of egg or sperm cells: one with the mutation and one without it. These mutations are rare, so it is highly unlikely that a person will have a mutation in the same gene on both chromosomes.

Therefore, there is a one out of two or 50% chance that each child will receive the mutation and a 50% chance that the child will not receive it. However, not everyone who inherits one of these mutations develops cancer. Inheriting a mutation means that the risk is increased, but not certain. Those who do develop cancer can be diagnosed from very young to older ages.
Sometimes individuals who have been diagnosed with cancer think that their genes must be "weaker" or "not as good" as those of other people. Actually, all human beings carry from five to fifty mutations that could cause illness or a physical problem. In some cases, one of these mutations is known or is apparent, but that does not mean the person has more mutations than someone else does.
Genetic Testing
Back to the Table of Contents
When a family has several cases of cancer, and an increased hereditary risk seems likely, individuals sometimes have genetic testing to determine whether they have or have not inherited a mutation that increases cancer risk. Not all that inherit a mutation are at increased risk of developing cancer. Those who find that they have inherited a mutation will generally take greater precautions to find cancers at the earliest times. Some will decide to have prophylactic surgery. Individuals who learn that they have not inherited a mutation that increases cancer risk may still be diagnosed with cancer, so they need to realize that prudent follow-up is still needed.
Genetic testing is done on a small sample of a person's blood. If you think of a gene as a building, as shown in Figure 5, you can think of a mutation that increases cancer risk as a damaged room in a building. When a person has genetic testing, the laboratory in essence walks through the building (gene) looking for a damaged room. At the present time many, but not all, mutations that increase cancer risk can be detected. So, if a person is tested and found to have a mutation, we know that the risk of cancer (and perhaps several cancers) is increased.

Once a mutation has been identified in an individual, his or her relatives can be tested to see if they have inherited the same mutation. Since mutations are rare, when the relatives of a person with a mutation are tested, it usually is not necessary to walk through the entire building again looking for other mutations. Instead, the laboratory looks only for the already detected damaged room.
Individuals of Ashkenazi Jewish descent who have BRCA testing are generally tested for mutations in three different locations or rooms, even if their relative has already been found to have a mutation, since it is relatively easy and inexpensive for scientists to look in these three locations. Some have heard that this group has a high BRCA mutation rate. They are surprised to learn that BRCA mutations are present in less than 2% of the Ashkenazi population.
If an individual with cancer is tested and no mutation is found, there are several possibilities:
- No mutation that increases cancer risk is present in the family so the individual did not inherit one and therefore cannot pass it on to his or her children.
- A mutation that increases cancer risk is present in the family, but this individual did not inherit it. That person's cancer is not due to strong hereditary factors, so the children cannot inherit a mutation that increases cancer risk from this person.
- A mutation that increases cancer risk is actually present in this individual, but it is not a mutation that can be detected with current scientific methods. In this case it does not make sense to test a person's children unless the other parent's family history suggests an increased cancer risk. Testing at a future time may be useful, however, since new mutations are being discovered with great regularity.
Who should have genetic testing? Since most cancers are not due to strong hereditary factors, most people decide to have testing only if they have a suspicion that hereditary factors are involved. Cost is also a consideration. Insurance companies are increasingly likely to pay for testing, but do not always do so. Some people are concerned about the insurance ramifications to individuals without a cancer diagnosis if a mutation is found in a family. To date, discrimination by insurance companies has been hard to document. Many states now have laws prohibiting discrimination on the basis of genetic test results, but disability and life insurance are not regulated at present. Insurance companies can simply ask about family history, and so use these criteria instead of testing, if they are truly concerned about insuring the relatively few people with strongly inherited cancer.
A final consideration in deciding to be tested has to do with the likelihood that the test result will enhance a person's emotional well being or help in making a health care decision. For example, a woman with a diagnosis of breast cancer may be concerned about knowing whether her risk of ovarian cancer is also increased. Or, that woman's daughter may want to know "for sure" whether she does or does not carry the mutation that was found in her mother. If she has not inherited it, she will feel secure having the check-ups recommended for the general population. And, she is likely to have fewer concerns about cancer. On the other hand, if she is found to carry a mutation, she is likely to intensify the type of medical care she receives.
In deciding whether genetic testing is for you, it is important to talk it over with an expert who specializes in cancer genetics. The field is changing so rapidly that only these experts are likely to have all the latest, most up to date information about testing and its ramifications.

Figures are from Assess Your True Risk of Breast Cancer Cancer by Patricia T. Kelly (Henry Holt and Co., NY) 2000
|
You are welcome to share this © article with friends, but do not forget to include the author name and web address. Permission needed to use articles on commercial and non commercial websites. Thank you. |
||